A rare autoimmune disorder destroyed the cartilage and bone in a woman’s nose, causing her nose to collapse and sag in her face.
When the 34-year-old woman went to a facial surgery clinic for plastic surgery, her nose bride completely collapsed, causing the tip of her. nose to withdraw, according to a report published on April 5 The New England Journal of Medicine (NEJM). The deformity arose over the course of seven years.
The woman had a variety of related symptoms, including persistent infection in her nasal cavity and the lining of her sinuses, a condition called ‘chronic rhinosinusitis’, and she also had fleshy growths in her nasal cavity known as ‘polyps’. A thin mucus leaked from her nose and a dry, bloody mucus formed over the inside of her nose.
Related: 27 strangest medical cases
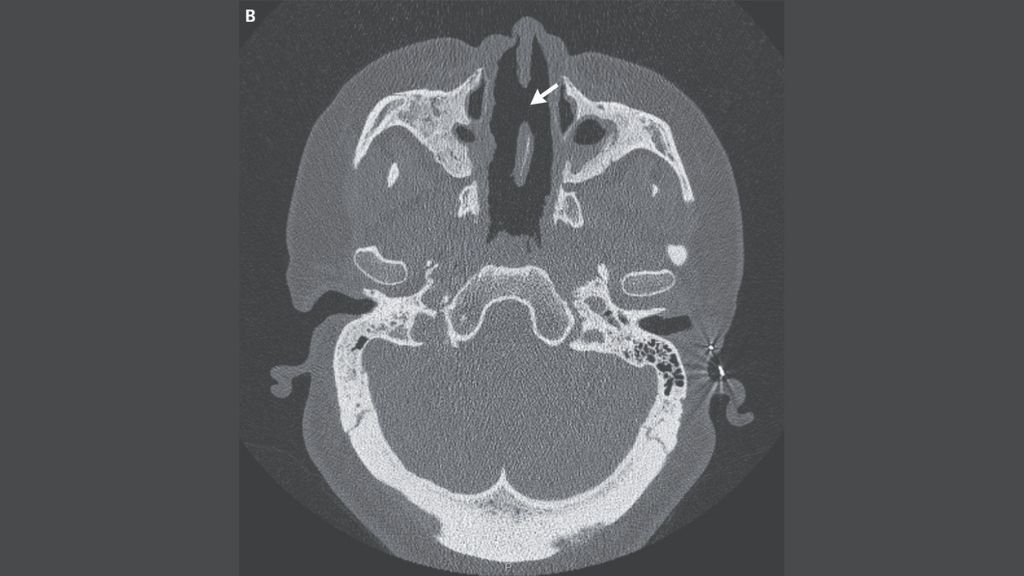
A physical examination showed an ‘almost total loss’ to the woman’s nose well, on either side of the bridge, and severe deterioration of her septal cartilage. In addition, a CT scan showed that a large hole had formed in the septum.
To investigate the cause of the turbulent inflammation, the doctors performed a test to identify it antibodies circulating in the woman’s blood. They found high levels of antibodies targeted at proteinase 3 (PR3), a protein found in certain white blood cells. according to the Mayo Clinic Laboratories. Antibodies targeting PR3 are a type of motor body, which means they attack healthy human cells, which can cause inflammation blood vessels and causing organ damage, mostly to the kidneys, longe and respiratory tract.
Based on the presence of PR3 antibodies in the woman, the doctor diagnosed her with ‘granulomatosis with polyangiitis’, or GPA. According to Mayo Clinic, almost all people with GPA carry these motor vehicle bodies.
That said, “the exact role that these motor road bodies play in the development of granulomatosis with polyangiitis is not fully understood,” according to the National Organization for Rare Disorders (NORD). One possibility is that these antibodies can cling to white blood cells carrying PR3 and somehow cause them to function and damage healthy tissues.
“Estimates of the frequency of granulomatosis with polyangiitis vary widely, depending on the specific population being studied,” and according to NORD, doctors often do not recognize the disease. As a result, it is difficult to estimate how many people develop the disease each year, but it is considered very rare.
According to NORD, GPA can develop slowly over many months or start quickly within a few days. Symptoms vary greatly from person to person, but can affect organs throughout the body. For example, severe cases can lead to hearing loss, vision loss, kidney failure or cranial nerve damage if left untreated. The autoimmune disorder can also cause a persistent runny nose, nasal congestion, sinusitis and holes in the septum, as seen in the affected woman.
To treat the woman’s GPA, her doctors prescribed rituximab, an antibody treatment that targets immune cells, B cells, to reduce the body’s immune response according to Drugs.com. The patient also received low dose cyclophosphamide, another immunosuppressant, and prednisone, a corticosteroid which also reduces immune activity.
“At a follow-up visit 6 months later, the patient’s bloody nasal discharge and crusting were resolved,” according to the NEJM report. “The nasal formation is unchanged.” The patient is still receiving rituximab, but the report does not mention whether she will undergo surgery for her sunken nose.
Originally published on Live Science.