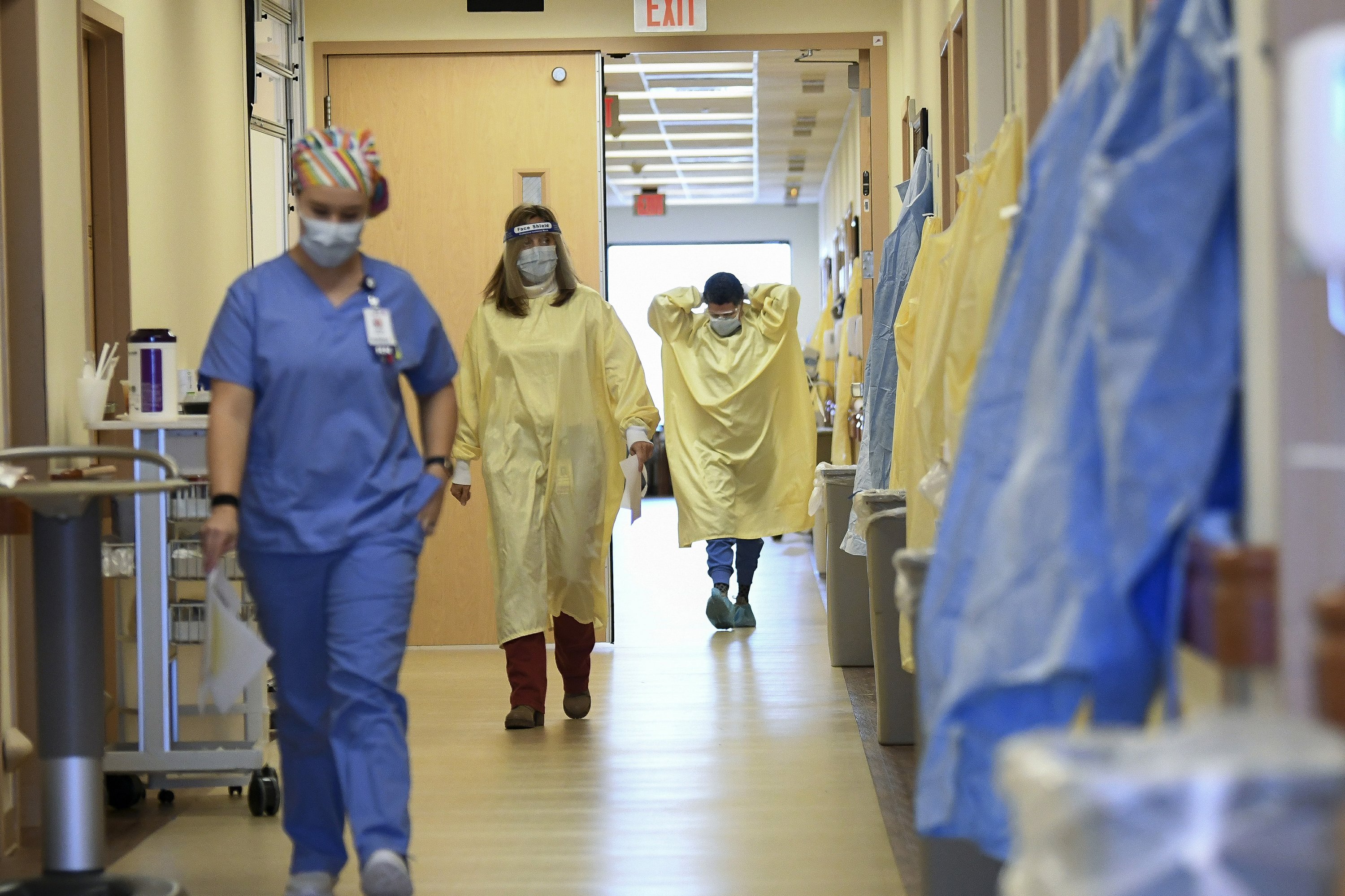
BIRMINGHAM, Ala (AP) – With its dozen intensive care beds already full, Cullman Regional Medical Center has begun desperately searching for options as more and more COVID-19 patients arrive.
Ten beds normally used for less severe cases have been converted into intensive care rooms, with extra IV machines brought in. Video monitors were set up to enable staff to monitor patients when a nurse had to scramble away to care for someone else.
The patch did the job – at least for now.
“We are similar to a bath that is full and the drain is blocked,” said the hospital’s medical chief, Dr. William Smith, said last week.
Alabama, long one of the most unhealthy and impoverished states in America, has emerged as one of the country’s most disturbing coronavirus hotspots.
Its hospitals are in crisis because the virus is raging out of control in a region with high obesity, high blood pressure and other conditions that could make COVID-19 even more dangerous, where access to health care was limited even before the outbreak, and where public resistance is stubborn against masks and other precautions.
The virus has killed more than 335,000 people in the United States, including more than 4,700 in Alabama. Places like California and Tennessee have also been hit particularly hard in recent weeks.
In Cullman Regional, a central hospital that serves an agricultural area 55 km north of Birmingham, the intensive care unit last week had 180% of capacity, the highest in the state. Other hospitals are also struggling to keep up with the pressure of people affected by the virus.
While a typical patient requires two or three days of ICU treatment, Smith said COVID-19 patients often stay two or three weeks, causing the case load to build up.
According to Johns Hopkins University, Alabama ranks sixth on the list of states with the most new cases per capita. Alabama’s latest average positivity rate – the percentage of tests positive for the virus – is nearly 40%, one of the highest in the country. And the state sees an average of 46 deaths a day, up from 30 on December 14
Although ICUs nationwide were at 78% in the week of Dec. 18-24, Alabamas were 91% full, according to the U.S. Department of Health and Human Services. Since last week, 15 Alabama hospitals have had intensive care units with a capacity or higher, and the ICUs at another six hospitals were at least 96% full.
On Monday, there were 2,800 people in Alabama hospitals with COVID-19, the highest total since the pandemic began.
Experts are worried that the stress will only increase after the holidays due to new infections related to travel and gatherings of family and friends.
“I think we are in a terrible state. I really do, ”said Dr. Don Williamson, head of the Alabama Hospital Association. “I’m afraid our Christmas boom is going to be a lot worse than the Thanksgiving boom.”
The Alabama government, Kay Ivey, at the time broke with some of its peers in South Africa and instituted a mandate for the entire machine that has been in place since July, but health officials have struggled to keep up with people. The Republican governor also issued a home order early in the pandemic, but strongly opposed it, saying, “You can not have a life without subsistence.”
In contrast, California has issued strict home orders in recent weeks in areas where ICU occupancy has reached 85%.
“Unfortunately, we have people who still gather in groups, travel for the holidays and do things that are unsafe,” said Dr. Alabama Health Officer Scott Harris said.
The deep-south state has some of the highest numbers of chronic health conditions that increase the risk of death or serious illness due to the coronavirus. Alabama has the sixth highest percentage of obesity in adults in the U.S. and is third in the percentage of adults with diabetes.
Alabama is also one of a dozen states that Medicaid has not expanded under the Affordable Care Act and therefore has a large number of uninsured. About 15% of people between the ages of 19 and 64 have no coverage, the 13th highest percentage in the country, according to the Henry J. Kaiser Family Foundation.
The state has closed 17 hospitals over the past decade, mostly small rural hospitals, a trend that has allowed local facilities to succeed.
At Decatur Morgan Hospital, COVID-19 deaths have tripled since September, and the intensive care unit is full, said Dr. James Boyle said. The pulmonologist struggled to maintain his composure and keep his lips still, while discussing the possibility of having to provide care in the new year.
‘I’m practicing in this country since ’98. “I have never had more than two or three people on ventilators with the flu in the last twenty years,” he said. ‘We always have a lot of patients in the ICU in the winter. Having 16 patients on ventilators with a disease we do not usually have is unprecedented. ”
UAB Hospital, affiliated with the University of Alabama in Birmingham, has brought in retired nurses and dozens of teachers and students from its nursing school to help.
Hospitals in Alabama receive calls from neighboring states like Mississippi and Tennessee, as doctors seek extra space for COVID-19 patients, but they may not be able to help as often as in the past. The same is true in the state, with hospitals that can help care for patients after a disaster like a tornado that cannot currently help.
With thousands of people already vaccinated with the first of the two doses needed to guard against COVID-19, the end of the pandemic is in sight. But the toll on medical workers is rising in the meantime.
“We see death. It is part of what we do; it is part of our training, ”said Boyle. ‘The problem this year is just the sheer number. We cannot grieve for one patient before we have to go to another. ”
___
Associated Press author Kim Chandler contributed to this story from Montgomery, Alabama.